Diverticulits:
therapy in Munich
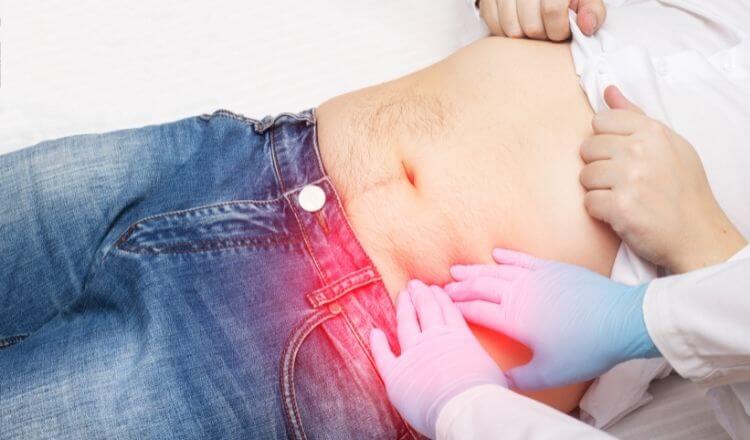
Diverticulitis is a digestive disease common in civilized countries. It is found particularly in the large intestine.
Diverticulitis develops from diverticulosis, the development of sack-like pouches or pockets (called diverticulum) on the outside of the colon due to internal pressure in the intestine. Diverticulitis is an acute inflammation of one or more of these diverticulum pouches or pockets.
The cause of diverticulitis is commonly ascribed to a diet low in fiber, lack of physical movement and exercise, congenital weakness of connective tissue, chronic constipation and genetic predisposition. Pressure in the colon causes sack-like pouches or pockets (diverticulum) to form on the outer surface of the intestinal wall. Fecal or undigested food matter such as nuts or seeds can become entrapped in the pouch causing inflammation (diverticulitis) possibly leading to infection and rupture of the colon wall (similar to appendicitis) possibly resulting in potentially fatal peritonitis. A second type of complication is if fecal matter entrapped in the diverticulum hardens and through natural movement of the colon rubs against the wall irritating it until inflammation occurs. This could lead to an ulceration of the diverticulum wall and inner bleeding of the colon.
A further complication occurs if the infected area sticks to another nearby organ such as the small intestine, bladder or ovaries. Tubular canals (called fistulae) can develop between those organs. A fistulae opening into the abdominal cavity will cause peritonitis resulting in death if untreated.
Another complication is obstruction of the bowels (ileus), through blockage, swelling of the intestines and eventual buildup of abscesses. In the worst case, this can lead to perforation of the intestinal wall with leakage of infected or fecal matter into the abdominal cavity and eventual peritonitis.
The most common location of diverticulum lies in the lower part of the larger intestine. Approximately 1/3 of patients who have developed diverticulum (diverticulosis) will also develop diverticulitis.
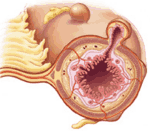
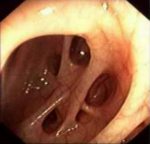
Approximately 1/3 of patients with diverticula will develop diverticulitis
Course of the disease mostly
symptomless
Conservative therapy
or surgery
Symptoms
Diverticulosis
Most people with diverticulosis do not have any discomfort or symptoms. Sometimes, symptoms that do occur may include mild cramps, bloating, and constipation interspaced with diarrhea. Occasionally, the diverticulum might bleed from irritation.
Diverticulitis
The most common symptom of diverticulitis is abdominal pain, especially in the left lower quadrant. This is accompanied by tenderness around the left side of the lower abdomen. If the diverticulitis has progressed to infection, fever, nausea, vomiting, chills, cramping, bleeding, constipation alternating with diarrhea will accompany the pain. The severity of symptoms will depend on the extent of the infection and other possible complications. A so called “diverticulitis tumor” may form and can be felt in the lower left abdominal quadrant. The pain can often extend to the bladder or kidneys and be confused with problems or diseases in these organs.
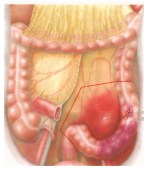
Diagnosis
The follow diagnostic procedures are used by suspicion of diverticular diseases (diverticulosis, diverticulitis):
- X-ray using a contrast agent
- Colonoscopy
- Ultrasound examination of the abdomen
- Lab examination of blood (for high white blood cells as an indication of infection)
- A computed tomography (CT) scan, if required.
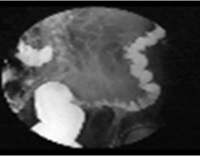
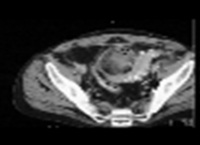
Therapy
Diverticulosis: Diverticulosis usually progresses without symptoms, and requires no medical therapy. Dietary restrictions, increased fluid consumption and increased fiber in the diet along with supplements are recommended to regulate bowel movement and alleviate discomfort.
Diverticulitis: Diverticulitis without complications can be treated with antibiotics and dietary measures to regulate bowel movement. Continuation of symptoms (chronic diverticulitis) and/or occurrence of complications are an indication that surgery is necessary to treat the disease.
Testimonial from a patient:
Very nice place, I had nice experience there with operation and the doctor is very careful and taking good care after my surgery.
Source: Google

Operation
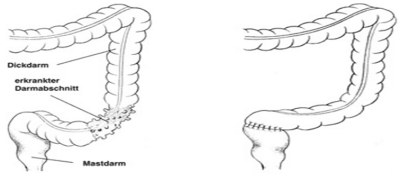
The procedure always involves removal of the area of the colon area with diverticulum (the part of the intestine covered with the sack-like pouches or pockets). Diverticulosis usually affects the sigmoid region of the colon, so the operation is called a sigmoid resection.
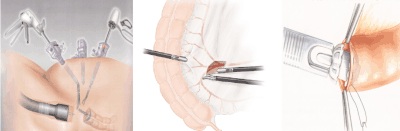
Minimal invasive Laparoscopic sigmoid resection:
A Laparoscopic sigmoid resection is a procedure using the laparoscope during a laparoscopy. In addition, several small incisions are made near the navel to insert other surgical instruments. The abdominal cavity is expanded with CO2 gas to improve camera perspective on the monitor and create more operating room. The sigmoid intestine with the diverticulum is cut and removed, and the wounds sutured.
The laparoscopic sigmoid resection is a gentler means of surgical removal of the infected intestinal region than open surgery. The wounds heal faster, normal diet can be restored quicker and overall recovery time is reduced.
Open surgery:
If laparoscopic sigmoid resection is not possible, for example due to scaring from previous operations, a conventional open abdominal incision (laparotomy) procedure can be used to remove the affected intestinal region.
Prognosis
Patients are usually released from the hospital 8-10 days after the operation, and can begin work after 3-4 weeks. The operation not only cures the acute diverticulitis, but also the diverticulosis: the intestinal region where the sack-like diverticulum develop, the sigmoid is removed thus ending further development. Dietary restrictions are emplaced until the intestines have regenerated and begun normal function again.
Notice: Preoperative preparation: Please inform your physician if you are taking blood thinning medication such as Aspirin® and Marcumar® as they may lead to complications during surgery. The intestinal tract will be emptied prior to the operation using a laxative or an enema.
Your health is
important to us
Office Hours
Monday, Tuesday, Wednesday: 8:30 – 16:00
Thursday: 8:30 – 18:00
Friday: 8:30 – 13:00
and by appointment
