Acid reflux, Gastroesophageal reflux disease (GERD)
Chronic acid reflux, (indigestion) properly termed gastroesophageal reflux disease (GERD) or [Br.E.] gastro-oesophageal reflux disease (GORD), is a disease due to abnormal reflux of stomach contents, chiefly stomach acid, into the esophagus causing chronic symptoms such as burning and damage to the mucosa lining of the esophagus.
Gastro-esophageal reflux disease is one of the most common benign diseases of the upper gastrointestinal tract in the western world. Some 10-25% of the population has some typical reflux symptoms such as “heartburn” or acidic regurgitation. The exact cause of acid reflux is not known, but gastro-esophageal reflux symptoms are commonly associated with hiatus hernia.
Acid reflux usually occurs due to weakness in the valve (termed the lower esophageal sphincter or LES) closing the stomach at the esophagus. If the valve does not close properly, stomach acid backs up into the esophagus causing a burning sensation behind the breastbone (sternum). GERD, Gastro-esophageal reflux disease, is the condition of chronic acid reflux into the esophagus. The esophagus eventually becomes inflamed (esophagitis). Some patients develop Barrett’s Esophagus (also called Barrett’s Epithelium or Barrett’s syndrome) when the cells lining the lower esophagus change abnormally so that they become columnar, resembling cells lining the stomach. While Barrett’s esophagus itself is a benign disease, it is often a preliminary stage to a carcinoma or esophageal cancer.
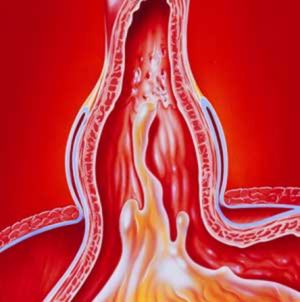
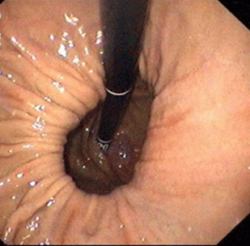
Other complications include peptic esophageal stenosis and esophageal ulcer both of which have the symptom of difficulty swallowing. These complications can be especially traced back to obesity, alcoholism, smoking, diet or congenital factors such as weakness in connective tissue building the esophageal sphincter.
Investigation using
gastroscopy
Conservative therapy
or surgery
Ability to work
10-14 days post op
Symptoms
Common symptoms of gastroesophageal reflux disease are chronic acidic regurgitation, heartburn, or a burning pain at the breastbone (sternum). If the esophagus is inflamed (reflux esophagitis) then further symptoms include difficulty swallowing, nausea, vomiting, regurgitation from partially digested food up to the throat and mouth (especially while lying down), coughing, choking, burping and pain in the upper abdomen.
Patients must be aware that the severity of the symptoms does not always correspond to the severity of the disease or inflammation. Scar tissue may develop at the critical point on the esophagus preventing strong pain despite the presence of strong inflammation. There is a 10% chance that chronic esophagitis develops into cancer.
Should the symptoms occur several times a week for 2-3 months, than the patient will require a gastroscopy to identify the cause of the symptoms and begin treatment.
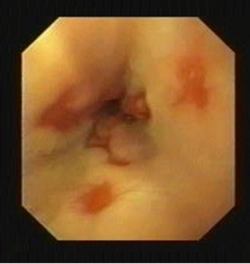
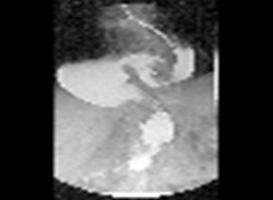
Diagnosis
There are several procedures used to diagnose gastroesophageal reflux disease and complications arising from it.
- Gastroscopy specifically called Esophagogastrodudenoscopy (EGD): This allows the physician to look at the affected areas (esophagus, stomach and duodenum).
- Abdominal sonogram: An ultrasound examination.
- Esophageal manometry measures the closing pressure developed by the lower esophagus sphincter.
- Esophageal ph monitoring over a 24 hour period measures acidity
- Barium radiocontrast swallow x-ray.
Testimonial from a patient:
Super friendly and helpful. Went there for a Gastroscopy and I was feeling very well taken care of, very calm environment and friendly staff! Me not speaking good German was not an issue what so ever.
Source: Google

Therapy
Conservative therapy
Operation: Laparoscopic antireflux surgery
Prognosis
Patients can usually leave the hospital 5-7 days after the operation, and can begin working after 10-14 days. The operation normally ends the acid reflux and relieves all accompanying symptoms. The laparoscopic procedures ensure that there are only small barely visible scars and that healing pain and healing time are reduced to a minimum. Because of the damage due to inflammation of the esophagus, the patient must return regularly for gastroscopy.
Notice: Preoperative preparation: Please inform your physician if you are taking blood thinning medication such as Aspirin® and Marcumar® as they may lead to complications during surgery.
Your health is
important to us
Office Hours
Monday, Tuesday, Wednesday: 8:30 – 16:00
Thursday: 8:30 – 18:00
Friday: 8:30 – 13:00
and by appointment
